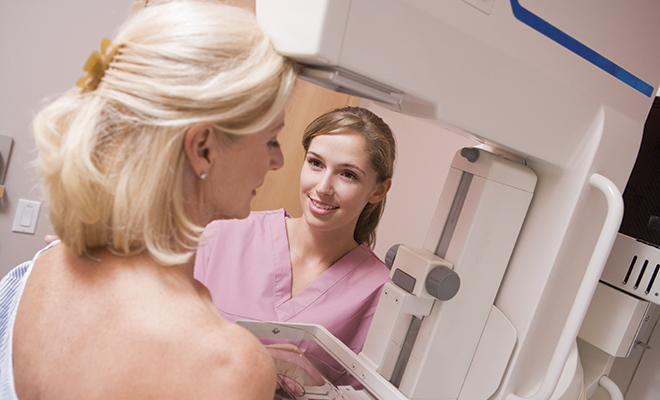
New Breast Screening Guidelines
It’s official. In May 2023, the U.S. Preventive Services Task Force, or USPSTF, issued new guidelines recommending that women begin having regular mammograms every two years starting at the age of 40 if they’re at average risk of breast cancer. That is a significant change from previous guidelines that women should be receiving routine mammograms at the age of 50.
This change comes after an increase in diagnoses of breast cancer among younger patients and a startling number of deaths among Black women, who are already 40 percent more likely to die of breast cancer. In addition, the task force now recommends women get screening mammograms every other year from ages 40 to 74.
What It Means
Each year, more than 43,000 women die of breast cancer in the U.S. The new guidelines would cover more than 20 million women between 40 and 49 who might be at risk, but women with a family history of genetic risk of breast cancer are advised to get screened earlier.
By amending its previous stance, the USPSTF’s is providing guidelines that are now more aligned with other groups’ recommendations. Other organizations including the American Cancer Society recommend women start screening or be offered the choice to start screening at age 40.
Why hasn’t there been consensus on screening guidelines in the past? While it has been an area of controversy many years, most experts say that the differing opinions of various organizations give varying, alternate perspectives that evaluate the benefits of screening versus the possibility of false positives and overtreatment.
Of course, the major benefit of screening is that it helps detect breast cancer sooner. When caught early, breast cancer, according to the American Cancer Society, has a five-year relative survival rate of 99 percent. Women with early-stage breast cancers generally need fewer and less-intense treatments and surgeries reach the five-year milestone.
On the other hand, screening does come with potential risks and harms. Although mammography is the best tool currently used, it is not perfect. Women can receive false positive results that require biopsies and additional imaging, which can cause unnecessary stress. Younger women tend to have dense breasts, which can make it harder to distinguish normal breast tissue from suspicious tissue, leading to more false positives as well.
Some experts disagree with the USPSTF’s recommendation that women get follow-up mammograms every other year from age 40 to 74. These screening guidelines are for women at average risk of developing breast cancer. The American Cancer Society, as well as other societies, still recommend annual screenings, and annual screening has been proven to lower the mortality rates. Having mammograms starting at age 40 should not change women’s insurance coverage. In the U.S., insurers are required to cover annual mammograms for women 40 and over.
Women who have a strong family history, particularly of early-age-onset breast cancer, younger than 45 years old, should discuss with their primary care doctor about the age to start having screening mammography. Experts say these groups should start having clinical breast exams at a much younger age, as young as 25, depending on the circumstances.
For women in their 40s who haven’t started screening, it’s best to talk to their medical provider about their own personal risk for breast cancer and schedule appointments as necessary. In addition, it’s important for a woman to know if she has dense breast tissue, which is crucial for overall breast health as she will likely need additional testing methods.
Higher-Risk Women
The American College of Radiology recommends women in higher risk groups, such as those of Ashkenazi Jewish descent and black women, get a breast cancer risk assessment by age 25, to determine if they need to start breast cancer screenings before age 40.
Women of Ashkenazi descent are more likely to carry the BRCA1 or BRCA2 breast cancer gene mutation, which raises their risk. It is still uncertain why black women are at increased risk for breast cancer, but what experts do know is that they present at a much younger age, and often with a more aggressive form of the disease. Survival rates are significantly worse than their white counterparts, with a 40 percent mortality rate stage for stage. Screening these women earlier will help save more lives, but tasks forces on this subject also note that more research is needed to determine if black women should be screened on an entirely different schedule.
Thankfully, the world of breast cancer detection is constantly evolving and growing. The updated recommendations emphasize the serious need to move from an age-based approach to breast cancer screening to a personalized, risk-based approach. This way, the research is focused on improving the assessment of the disease as well as the screening tools that are used to find it. ®
Sources: Sources: bcrf.org, cdc.gov, fox5atlanta.com and pbs.org.